TRILLIANT HEALTH RESEARCH
Research
Timely trend analysis. Free in your inbox.
Receive weekly studies from Trilliant Health.
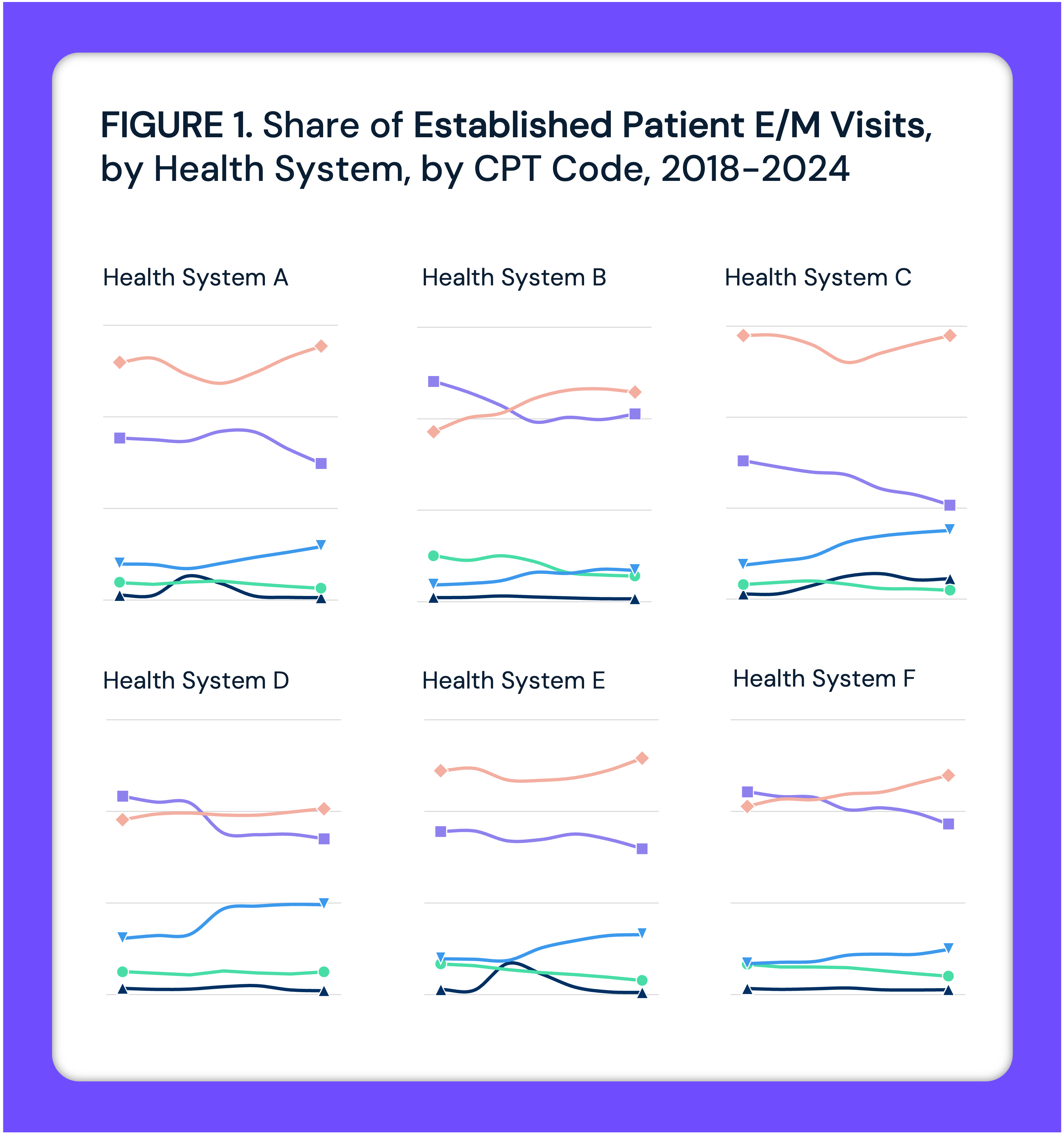
Increased Outpatient Coding Intensity Following Hospital Adoption of AI-Enabled Scribing Warrants Examination but Likely Reflects Enhanced Rules-Based Documentation
Read the StudyApril 30, 2026
The Majority of Hospital and Health Plan Reported Rates Diverge by More Than 10%
Less than half of hospital and health plan reported rates align with 10%; over 80% differ by more than 10%, with some diverging by over 17x, undermining price transparency and benchmarking.
Katie Patton
StudiesApril 23, 2026
As the Number of Residency Positions Increase in 2026, Primary Care Fill Rates Decline and Workforce Gaps Widen
2026 Match data shows increasing residency positions, but worsening gaps as primary care goes unfilled, signaling supply growth misaligned with workforce demand.
Clara Petrucelli
FundamentalsApril 21, 2026
The Demographic Composition of Local Markets Determines Localized Healthcare Demand
Demographic shifts – aging, declining births, slowing immigration – are reshaping U.S. healthcare demand unevenly across markets, demanding local analysis over national averages.
Clara Petrucelli
StudiesApril 16, 2026
Despite Behavioral Health Prescription Volume Growth, the Behavioral Health Treatment Gap Has Widened
Despite growing behavioral health prescriptions, the treatment gap widened – more patients go untreated (22.4% in 2024), stimulant use increased and allied health professionals now lead prescribing.
Katie Patton
FundamentalsApril 14, 2026
More Demand, Inadequate Supply, Higher Costs: An Examination of America’s Behavioral Health Crisis
Behavioral health demand is rising, the workforce is stretched thin and costs vary by as much as 7x for identical services. Trilliant Health's analysis, based on national claims data, reveals what's driving the gap.
Katie Patton
StudiesApril 09, 2026
Despite Growth in Genetic Testing, Fewer Than 20% of Mastectomy Patients Receive BRCA1/2 Testing Prior to Surgery
BRCA1/2 testing is increasing but still underused before mastectomy. Most patients have surgery without prior testing, missing chances for risk-informed decisions. Access and integration remain limited.
Katie Patton
StudiesApril 03, 2026
Hundreds of Hospitals Rely on Non-Patient Revenue to Maintain Positive Margins
Hospital revenue goes far beyond patient care. Discover how non-clinical income, labor costs and operating margins shaped the financial health of U.S. hospitals in 2024.
Katie Patton
StudiesApril 02, 2026
Behavioral Health Demand Is High and Increasing, With Growth Distributed Across a Wide Range of Diagnoses
Behavioral health visits increased 62.6% from 2018 to 2024, driven by anxiety and emotional disorders. Change in volume by diagnoses groups varies widely, suggesting more complex needs.
Clara Petrucelli
StrategyMarch 31, 2026
A Five-Year Strategy for Redesigning Employee Health Benefits to Compete in the Era of “Value for Money”
Price transparency will transform healthcare by enabling employers to save billions, improve quality and drive competition, as they steer employees to high-value providers using transparent data.
Clara Petrucelli






















.png)

















.png?width=171&height=239&name=2025%20Trends%20Report%20Nav%20(1).png)
