In our previous research examining provider prescribing patterns for certain opioids, we noted that nationwide pharmacy chains and digital pharmacies recently halted dispensing of controlled substances, particularly Adderall and its associated generics, from tele-enabled mental health apps.1,2,3 Over the last month, focus on this subject has intensified, leading to a Federal Trade Commission (FTC) investigation of the marketing practices of Cerebral, a company offering online treatment and medication management.4
The FTC investigation and continued scrutiny of tele-prescribing prompted us to analyze the extent to which diagnosing and prescribing patterns related to attention deficit/hyperactivity disorder (ADHD) changed over the last two years.
Background
The COVID-19 pandemic accelerated growth opportunities for digital health companies (e.g., e-prescribing), with over a quarter of the population using telehealth across 2020 and 2021.5 Additionally, the abrupt switch to remote work and school was reportedly associated with an increase in parents seeking ADHD treatment for their children.6
Researchers also have concluded that while telehealth poses significant opportunities for the diagnosis of ADHD, more evidence is required to determine the effects of long-term digital treatment and monitoring of ADHD.7 Additionally, other research has found that patients who were tele-prescribed antibiotics were more likely to rate their doctors five stars than those who did not, raising potential concerns over incentives for over-prescribing via telehealth platforms.8
While companies like Cerebral were well positioned to cover important gaps in in-person behavioral healthcare during the COVID-19 pandemic, their business model raised concerns of over-prescribing and inappropriate marketing tactics (e.g., advertising on the social media platform TikTok).
Analytic Approach
Using all-payer claims data, we examined ADHD-related medical encounters and prescriptions at the patient level between 2018 and 2021. Across payer types, patients were segmented by age (0-21, 22-44, 45+). We then examined quarterly trends in ADHD diagnoses and generic or brand-name Adderall prescriptions.
Findings
For children and young adults, patient volumes for ADHD and medication management were impacted by the pandemic, with patient volumes declining 13.9% and 15.6%, respectively, from Q2 2019 to Q2 2020 (Figure 1). Since Q4 2020, volumes and Adderall prescriptions for this age group have stabilized below pre-pandemic levels. Conversely, for patients ages 22-44, patient volumes and Adderall prescriptions increased in 2020 and 2021, compared to pre-pandemic years (Figure 2).
The number of patients in this age group with Adderall prescriptions increased 7.4% from Q2 2019 to Q2 2020, followed by a 15.1% increase from Q2 2020 to Q2 2021. In contrast, patient volumes for the 45+ age cohort remained relatively stable year-over-year, with a slight uptick in prescription volumes in 2021.
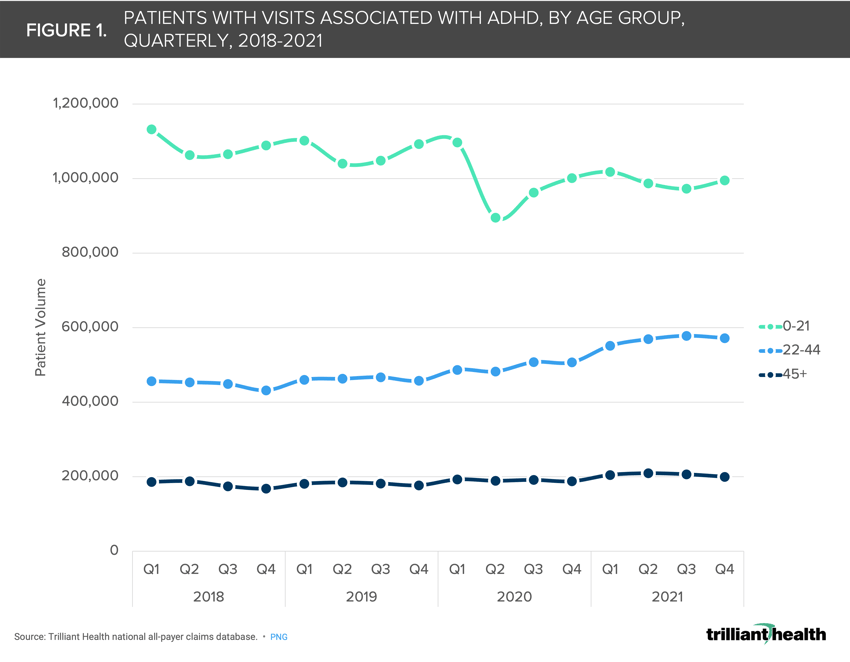
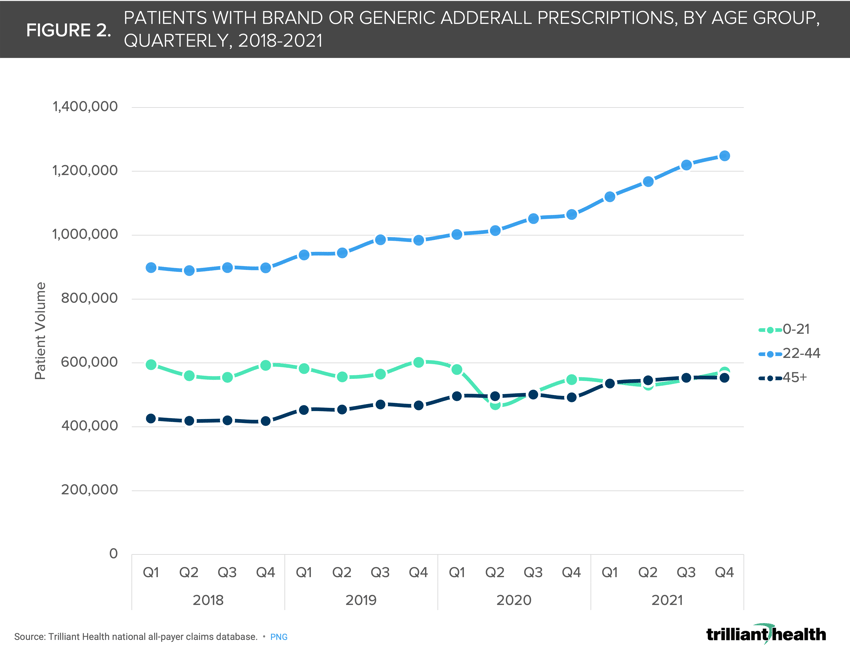
In hindsight, it is clear that the emergence of digital mental health platforms enabled significant increases in prescribing, particularly for the Millennial generation. Notably, there are more adults receiving prescription Adderall than there are with a formal ADHD diagnosis. This discrepancy likely speaks to the number of individuals using a direct-to-consumer, self-pay service in this clinical scenario.
In contrast, despite flawed reports of increased ADHD diagnosis and treatment for adolescents amid remote schooling, patient volumes for children and young adults dropped from Q1 2020 to Q2 2020. Remote learning is one possible explanation for this decline, given ADHD often is first observed by teachers and counselors in the in-person school setting.
Due to a confluence of events, the standard approach to the diagnosis and treatment of ADHD was undeniably altered during the pandemic. As more evidence becomes available, it is more than likely similar trends will reveal themselves across a variety of clinical scenarios.
Thanks to Kelly Boyce and Katie Patton for their research support.