TRILLIANT HEALTH RESEARCH
Research
Timely trend analysis. Free in your inbox.
Receive weekly studies from Trilliant Health.
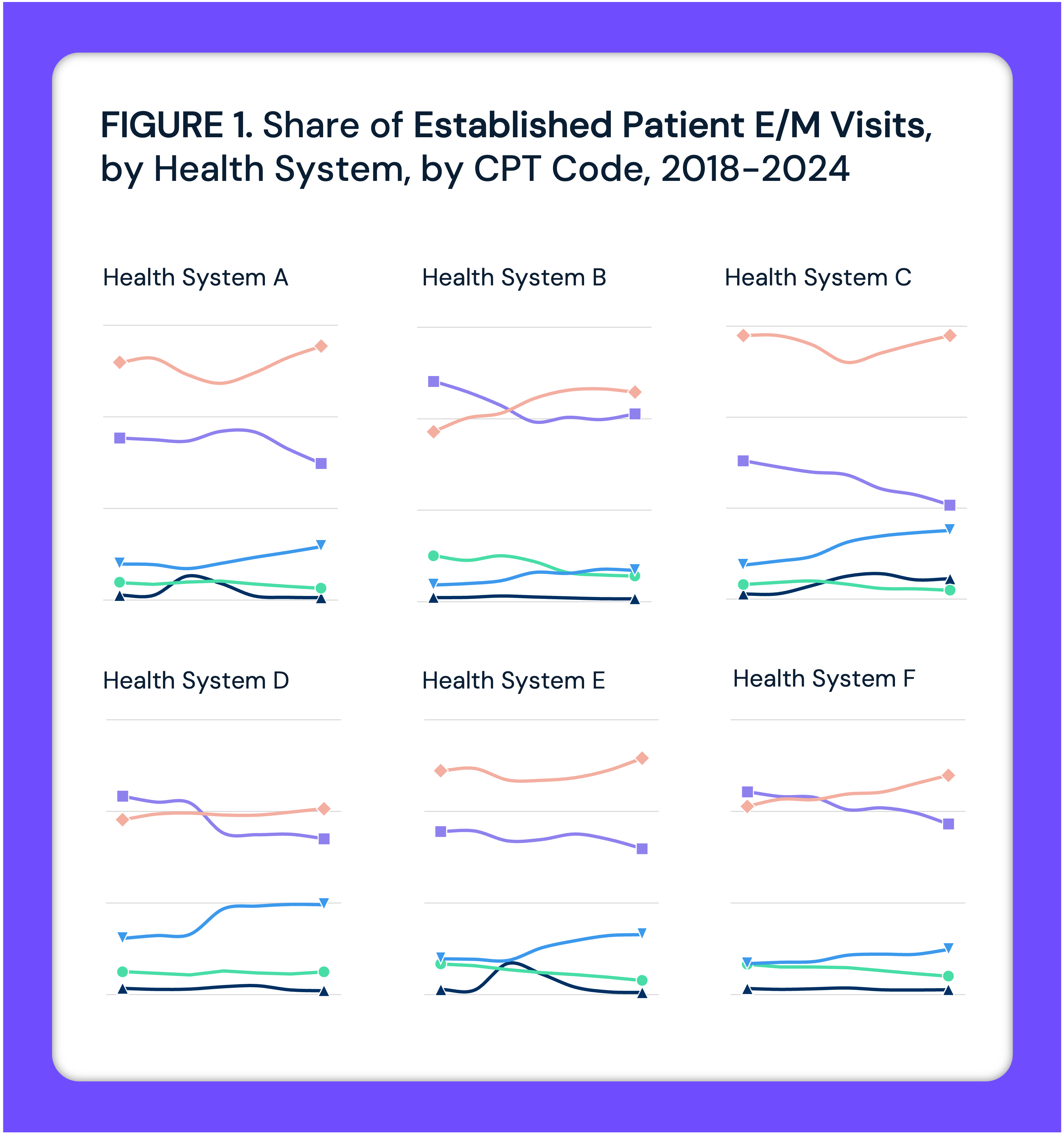
Increased Outpatient Coding Intensity Following Hospital Adoption of AI-Enabled Scribing Warrants Examination but Likely Reflects Enhanced Rules-Based Documentation
Read the StudyApril 03, 2026
Hundreds of Hospitals Rely on Non-Patient Revenue to Maintain Positive Margins
Hospital revenue goes far beyond patient care. Discover how non-clinical income, labor costs and operating margins shaped the financial health of U.S. hospitals in 2024.
Katie Patton
StudiesApril 02, 2026
Behavioral Health Demand Is High and Increasing, With Growth Distributed Across a Wide Range of Diagnoses
Behavioral health visits increased 62.6% from 2018 to 2024, driven by anxiety and emotional disorders. Change in volume by diagnoses groups varies widely, suggesting more complex needs.
Clara Petrucelli
StrategyMarch 31, 2026
A Five-Year Strategy for Redesigning Employee Health Benefits to Compete in the Era of “Value for Money”
Price transparency will transform healthcare by enabling employers to save billions, improve quality and drive competition, as they steer employees to high-value providers using transparent data.
Clara Petrucelli
StudiesMarch 26, 2026
GLP-1 Therapy Growth Has Reshaped Anti-Obesity Prescribing
GLP-1 therapies are replacing older anti-obesity drugs, driven by higher efficacy and patient demand – but costs, coverage, adherence and long-term effectiveness remain key challenges for broad adoption.
Katie Patton
StudiesMarch 12, 2026
Increased Outpatient Coding Intensity Following Hospital Adoption of AI-Enabled Scribing Warrants Examination but Likely Reflects Enhanced Rules-Based Documentation
Adoption of AI-enabled scribing in hospitals increased outpatient coding intensity, likely due to more accurate documentation, raising questions about impact on billing, reimbursement and fraud risks.
Katie Patton
StudiesMarch 05, 2026
As RPM Growth Slows, Medicare Expands Coverage While Commercial Insurers Question Effectiveness
RPM growth has slowed, with Medicare expanding coverage, but commercial insurers restricting requirements due to mixed evidence of effectiveness, concentrating use in cardiovascular and metabolic cases.
Katie Patton • Austin Miller • Allison Oakes, Ph.D.
FundamentalsMarch 03, 2026
Examining CMS’s National Health Expenditure Estimates for 2024
U.S. healthcare spending keeps rising, driven by higher prices, shifting care to outpatient settings and greater treatment intensity, even as overall care utilization remains flat or declines.
Clara Petrucelli • Katie Patton • Allison Oakes, Ph.D.
StudiesFebruary 26, 2026
Cancer Survival Up 140% Since the Mid-1970s, but Mortality Improvements Are Uneven Across Racial Groups
ACS projects 2.1M new cancer cases and 626,140 deaths in the U.S. for 2026. Five-year survival has reached 70%, but disparities persist by race, region and socioeconomic status.
Clara Petrucelli • Katie Patton • Allison Oakes, Ph.D.
StudiesFebruary 19, 2026
Intra-Market Rate Variation Can Lead to Spending Differences that Exceed $102M for a Single Orthopedic Procedure in Dallas-Fort Worth
Health plan price transparency data reveals notable price variation for the same procedures, enabling employers to cut costs by steering employees to high-value providers and optimizing network choices.
Katie Patton • Jim Browne • Chris Rash • David Taylor • Allison Oakes, Ph.D.






















.png)

















.png?width=171&height=239&name=2025%20Trends%20Report%20Nav%20(1).png)
