Studies Archive
More Anxiety and Depression Patients Seeking Psychotherapy Following the Wake of the Pandemic
June 12, 2022Recently, we explored how, despite increased levels of investment activity in behavioral health, a long-term mismatch between supply and demand for behavioral health services will affect many stakeholders in the health economy. 1 Volumes for behavioral health across sites of care (i.e., telehealth, emergency department) continue to be substantially higher than pre-pandemic levels and show no signs of abating in the near term. Yet less is known about the pandemic’s impact on the treatment trends (e.g., no treatment, psychotherapy, pharmacotherapy) for anxiety and depression.
Background
Demand for treatment of depression increased 58% in 2020 and 70% in 2021, while demand for treatment of anxiety increased 72% and 82% in the same time periods, according to the American Psychological Association.2 Substantial research has been published on the pandemic’s impact on the nation’s mental health status, particularly regarding acute anxiety at the pandemic's onset in 2020.3,4,5
As treatment demand for anxiety and depression and the availability of virtual care options have simultaneously increased, the extent to which treatment patterns have changed are unknown. Current practice guidelines recommend a combination of psychotherapy and pharmacotherapy (also referred to as medication management) for depression and severe anxiety, but patient preference for and availability of different treatment options inevitably influences the course of treatment.6,7,8,9,10,11
Analytic Approach
To assess the pandemic’s impact, we investigated the magnitude of treatment shifts (i.e., psychotherapy and medication management) between 2019 (pre-pandemic) and 2021. We identified adult patients ages 18-64 across payer types between 2019 and 2021 with diagnoses of either anxiety or depression. We then segmented these patients by year of diagnosis to determine changes in treatment of those diagnoses. In each year, we determined the proportion of patients that (i) received a diagnosis but did not treat with psychotherapy or medication management, (ii) received psychotherapy treatment only, (iii) were treated with medication management only, or (iv) received psychotherapy and medication management. Notably, patients receiving psychotherapy or medication management through self-pay arrangements are not reflected in the analysis, as it is claims based.
Findings
Between 2019 and 2021, the number of patients diagnosed with depression or anxiety increased by 11.1% from 9M to 10M. Across this time period, there was almost no change in the proportion of patients diagnosed with either anxiety or depression who did not seek treatment. A higher proportion of patients are treating with psychotherapy alone or in combination with medication management. The proportion of patients solely treating with medication management declined annually in the observed timeframe.
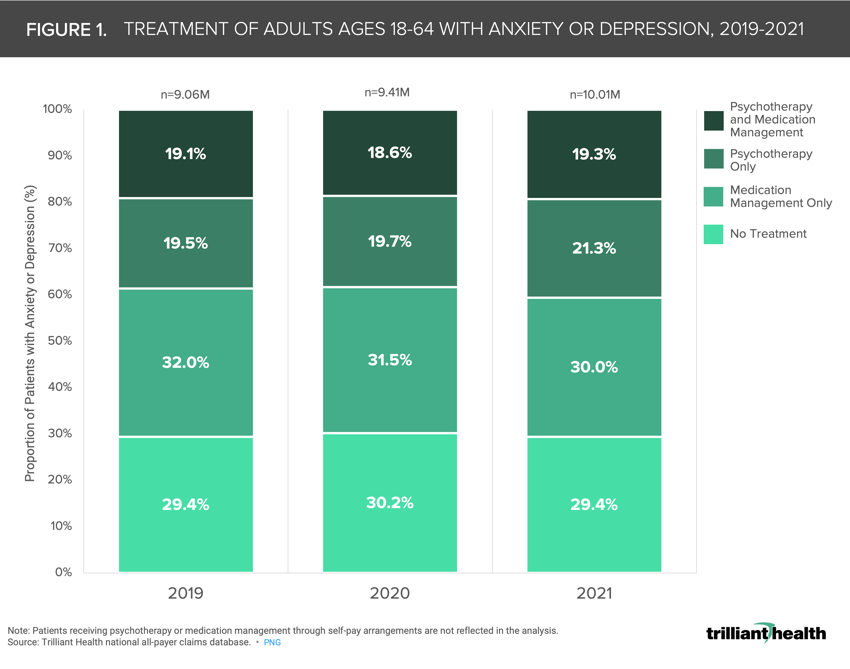 Notably, 2% of patients (totaling over 150K) that solely treated their anxiety or depression with psychotherapy throughout 2019 added medication management to their treatment regimen in 2020 or 2021, suggesting severity of diagnosed disorders could have been exacerbated by the pandemic.
Notably, 2% of patients (totaling over 150K) that solely treated their anxiety or depression with psychotherapy throughout 2019 added medication management to their treatment regimen in 2020 or 2021, suggesting severity of diagnosed disorders could have been exacerbated by the pandemic.
While the volume of patients increased in each category of the analysis, it is notable that the proportion of patients being treated with psychotherapy increased, while the proportion solely using medication management declined. The increase in tele-enabled therapy platforms likely provided better access than traditional in-office psychotherapy. As we previously found, behavioral and mental health conditions were the most common telehealth use case during the pandemic (57.9% of all telehealth visits).12 Additionally, the pandemic introduced challenges and uncertainty universally, leading to extensive societal focus on mental health, perhaps lessening existing stigma related to seeking mental and behavioral health treatment via psychotherapy.
In next week’s analysis, we will dive deeper into how trends in the treatment and diagnosis of attention-deficit/hyperactivity disorder changed across age groups, both juvenile and adult, in the wake of the COVID-19 pandemic.
Thanks to Kelly Boyce and Katie Patton for their research support.























.png)

















.png?width=171&height=239&name=2025%20Trends%20Report%20Nav%20(1).png)




