Key Takeaways
-
Adolescents are being diagnosed with significantly more behavioral health conditions (e.g., eating disorders, depression) since the onset of the pandemic.
-
Overall, patient volumes for anorexia nervosa have been increasing at a faster rate than all other eating disorders for both children and adolescents (ages 0-17) and adults (ages 18+) since the onset of the pandemic.
-
Patient volumes for anorexia nervosa were up 101.4% in Q2 2022 compared to Q1 2018 for patients ages 0-17, and 48.1% for adult patients.
As federal and state government agencies begin to unwind temporary policies implemented under the public health emergency (PHE) expiring on May 11, 2023, the state of Americans’ mental health status has been, in many ways, irreparably changed by the COVID-19 pandemic. Notably, adolescents are being diagnosed with substantially more behavioral health conditions (e.g., eating disorders, depression) since the onset of the pandemic. The long-term effects of the pandemic on this cohort are not fully known and require attention from stakeholders across the health economy.
Background
Hospitalizations for eating disorders spiked during the pandemic, doubling among females ages 12-17. This increase was likely exacerbated by pandemic-related risk factors such as lack of structure in daily routine, emotional distress, changes in food availability or reduced access to mental health care in light of growing demand for services.1,2 Other research examining trends at a subset of academic adolescent medicine sites found increases in both inpatient and outpatient demand for eating disorder treatment after onset of the pandemic.3
The growth in adolescent behavioral health diagnoses occurred in parallel with increased social media adoption. Visits for eating disorders, depressive disorders and self-harm among patients below age 18 increased at rates higher than the overall population since the onset of the pandemic (Figure 1).
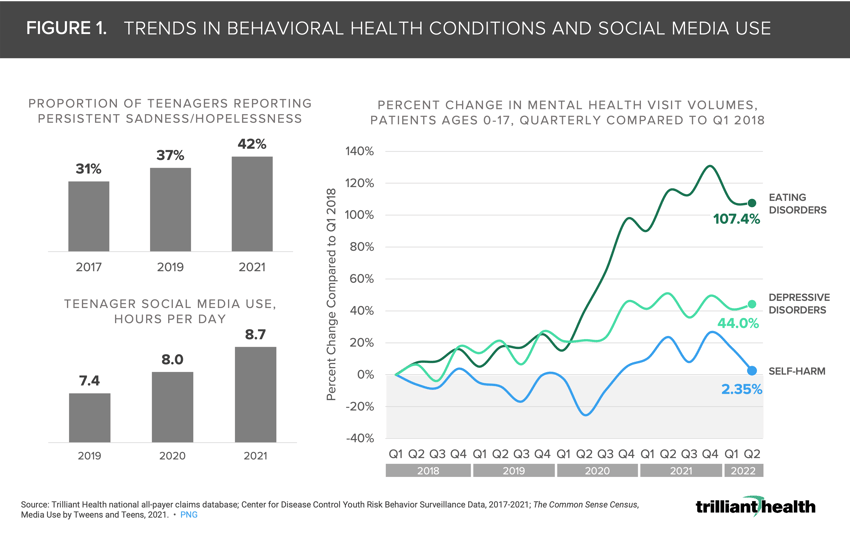
In order for clinicians and public health experts to implement effective interventions and preventive measures, more research is needed to understand the national-level change in eating disorders since the onset of the pandemic.
Analytic Approach
We studied patients with inpatient and outpatient medical encounters for eating disorders quarterly between Q1 2018 and Q2 2022. Patients were segmented into two age cohorts (ages 0-17 and ages 18 and older) and two diagnoses cohorts comparing anorexia nervosa to all other eating disorders (e.g., binge eating disorders, bulimia nervosa). To understand the magnitude of change in patients treated over time, the number of patients treated quarterly were compared to the volume of patients in Q1 2018.
Findings
Overall, patient volumes for anorexia nervosa have been increasing at a faster rate than all other eating disorders for both children and adolescents (ages 0-17) and adults (ages 18+) since the onset of the pandemic in Q2 2020. Patient volumes for anorexia nervosa increased 101.4% in Q2 2022 compared to Q1 2018 for patients ages 0-17, and 48.1% for adult patients (Figure 2). For all other eating disorders, patient volumes increased 85.3% and 45.6%, respectively, in the same time period. Consistent with other research, females accounted for the majority of patients across age groups—74.0% of patients ages 0-17, 88.3% of patients ages 18-44, 82.2% of patients ages 45-64, and 74.7% of patients ages 65+.
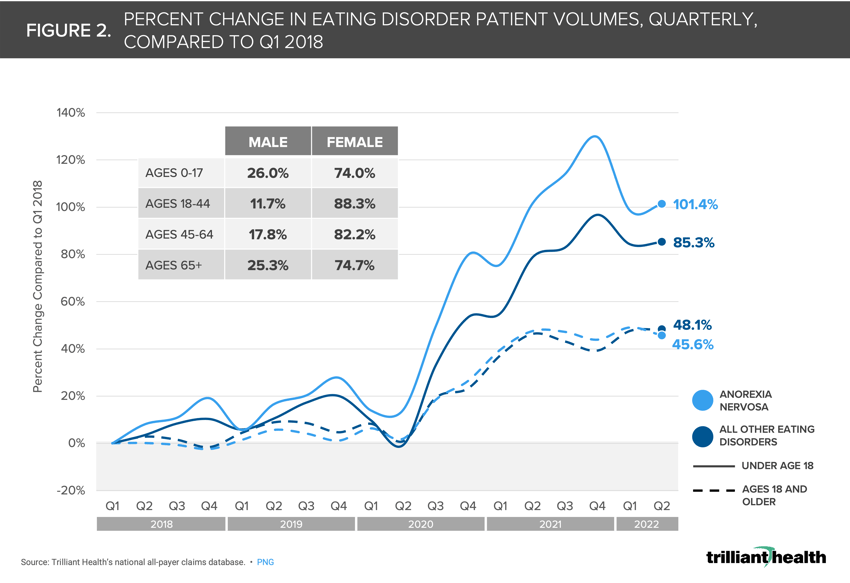
The response to the pandemic exacerbated social isolation and introduced disruptions to daily routines and structure, particularly for children and adolescents. Perhaps not surprisingly, the return to daily routines of school and extracurricular activities is not reflected in improved behavioral health, as patient volumes for eating disorders, especially for adolescents, have continued to increase. To what extent this sustained rise in eating disorders may be correlated with the growing off-label use of certain drugs for weight loss is not yet known. The fact that patient volumes appear to have normalized well above pre-pandemic levels and external risk factors (e.g., social media use, reduced access to behavioral health providers) persist should concern all stakeholders in the health economy.
Effective interventions require a precise understanding of these patient cohorts, including their psychographic profile and longitudinal healthcare interactions, to inform their healthcare decision-making process and likely adherence to treatment recommendations. If these interventions fail, younger patients can be expected to experience additional higher-cost comorbid behavioral and physical health conditions, which in turn are likely to extend into their adulthood. Such an outcome will only amplify America’s healthcare crisis.