Studies Archive
Evolving Emergency Department Utilization Signals Emerging Patient Needs
February 18, 2024Key Takeaways
- Analysis of emergency department (ED) visits from 2017 to 2022 revealed notable shifts in diagnosis patterns across age groups. While respiratory conditions gradually declined as a share of ED visits, circulatory and genitourinary conditions increased slightly.
- The observed trends in ED utilization reflect evolving disease burden and service demand and highlight the importance of adapting healthcare strategies to address emerging public health challenges.
- Understanding evolving trends in healthcare demand is important to inform resource allocation, preventive measures and healthcare policy aimed at improving patient outcomes.
- While no singular trend is driving changes in ED utilization over time, cardiac, behavioral health and genitourinary conditions have seen an increase in their share of ED visits, while the share of respiratory conditions in the ED has declined.
February is American Heart Month, which recognizes heart disease as the nation's leading cause of mortality – accounting for one in five deaths annually.1,2
From a policy perspective, investing in preventive care and health promotion is important to mitigate the growing burden of disease nationally. From an operational perspective, understanding the settings of care in which acute cardiac patients are treated – notably the emergency department (ED) – is essential for resource allocation.
Our 2023 Health Economy Trends Report noted a slight increase in overall ED volumes from 2021 to 2022, underscoring the importance of knowing who is receiving care in the ED and what for. National hospital spending was $1.35T in 2022, and more than half of hospital admissions originate in the ED.3
Because of the cost and policy implications of ED utilization, we examined changes in ED utilization over time, analyzing the composition of cardiac demand and the most common diagnoses in the ED.
Background
Insight into historic ED demand provides context for interpreting certain challenges within the healthcare system. Various factors have influenced the utilization of ED services over time, including shifts in population demographics, advances in medical technology and changes in healthcare policy, most notably the Emergency Medical Treatment & Labor Act (EMTALA). EMTALA, enacted in 1986, ensured public access to hospital-based emergency services regardless of ability to pay.
Despite numerous initiatives to alleviate strain on hospital EDs by establishing alternative non-emergent sites of care like urgent care facilities, retail care clinics and telehealth, concerns of overutilization persist.4,5 Longstanding efforts to address ED utilization were undermined in 2020 by policy decisions during the COVID-19 pandemic and have been exacerbated by the nation’s ongoing behavioral health crisis.
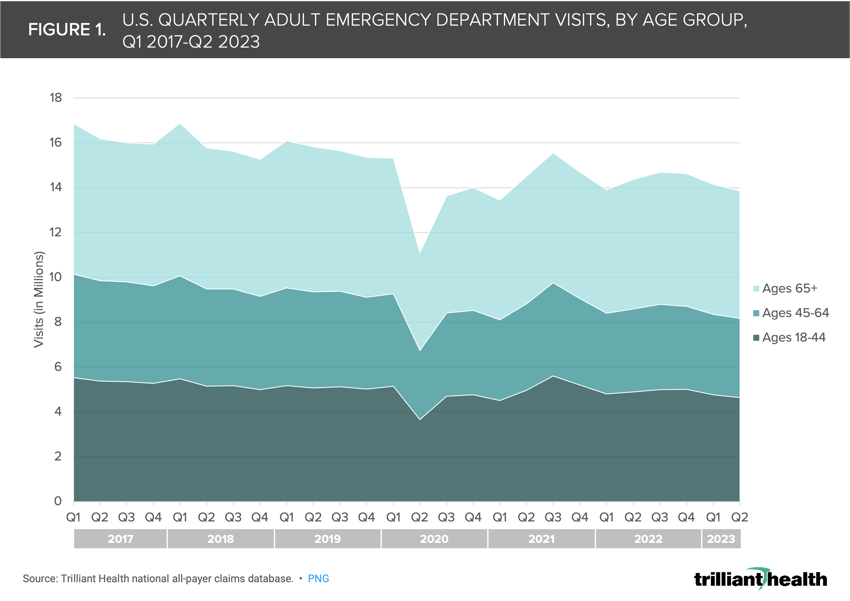
Overall adult ED utilization has trended slightly downwards compared to pre-pandemic averages. From 2017 to 2019, annual adult ED volumes declined slightly with an average annual growth rate of -2.7% (Figure 1). However, in 2022, volumes were 8.5% below utilization in 2019. By age, utilization has most closely rebounded to pre-pandemic levels for patients ages 18-44, down 3.3% from 2019 to 2022. In contrast, 2022 utilization declined 13.0% and 9.5% from 2019 for patients ages 45-64 and over 65, respectively.
Despite this national trend, changes in ED utilization vary substantially by both region and individual hospital. While national volumes have gradually trended downwards, we were interested in examining changes in the distribution of visits by reason (e.g., cardiac, respiratory, behavioral health) over time.
Analytic Approach
We utilized national all-payer claims to examine the annual distribution of adult (ages 18+) ED visits according to major diagnostic category (e.g., conditions of the circulatory system, digestive system) from 2017 to 2022, both in aggregate and within distinct age bands – ages 18-44, 45-65 and 65+.
Visits coded as “Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified (ICD-10 R00-R99)” were not included in this distribution. This chapter of ICD-10 codes includes symptoms, signs, abnormal results of clinical or other investigative procedures and ill-defined conditions regarding which no diagnosis classifiable elsewhere is recorded.
Additionally, we conducted an analysis of the most common diagnoses in the ED annually, both for all causes and specifically for conditions of the circulatory system.
Findings
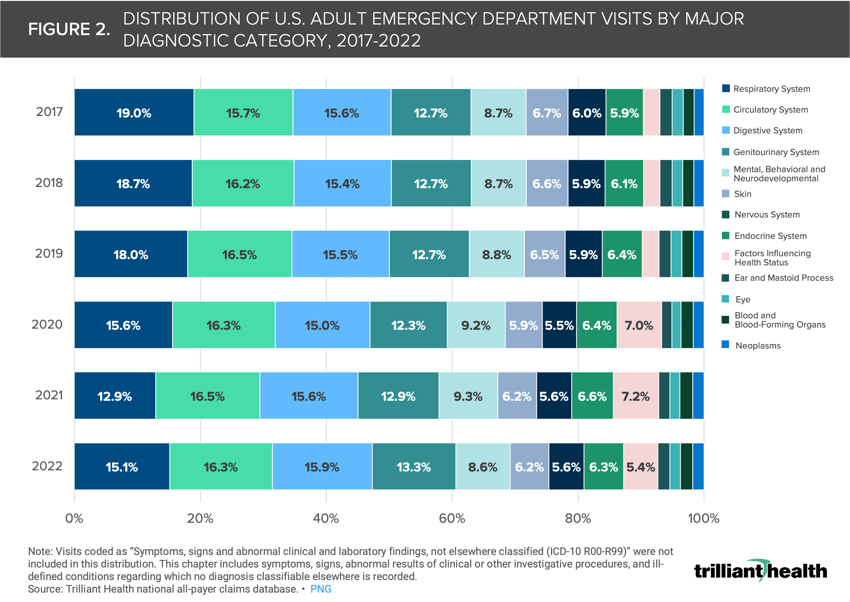
Respiratory ED visits experienced a gradual decline from 19.0% in 2017 to 12.9% in 2021 before increasing to 15.1% in 2022 (Figure 2).
Conversely, circulatory ED visits increased slightly from 15.7% in 2017 to 16.3% in 2022. ED visits related to genitourinary system also increased slightly from 12.7% in 2017 to 13.3% in 2022.
Digestive ED visits ranged from 15.0% to 15.9% throughout the period analyzed.
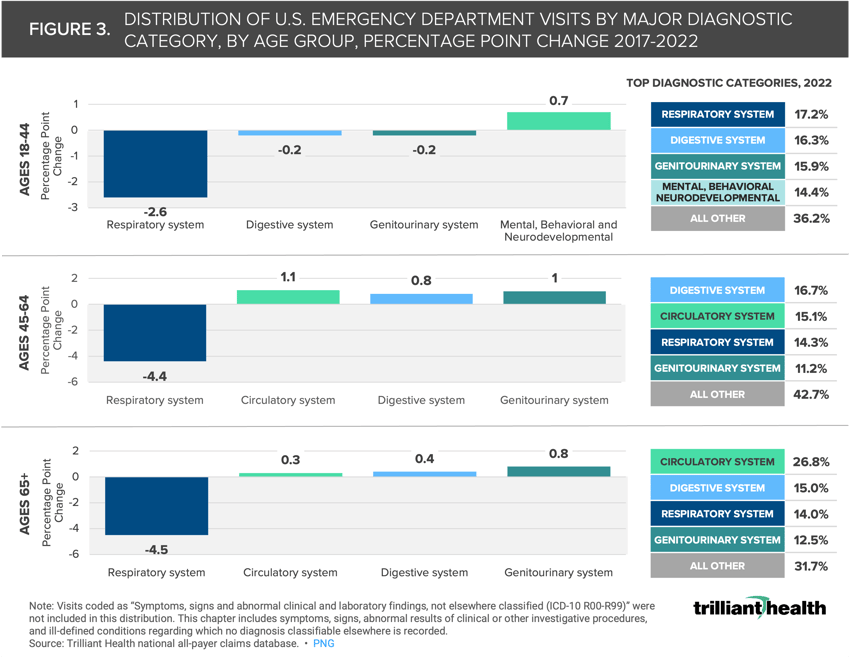
As expected, the proportion of visits attributed to general factors influencing health status (e.g., COVID-19) increased most from 2017 to 2022: +3.8, +2.7 and +2.2 percentage points (PP) for patients ages 18-44, 45-64, and 65+, respectively (Figure 3).
Similarly, the share of circulatory visits also increased across age bands: +0.5, +1.1 and +0.3 PP, respectively.
In 2022, respiratory ED visits represented the highest share of visits for patients ages 18-44 (17.2%) yet decreased in overall share by 2.6 PP from 2017 to 2022.
Conversely for patients ages 45-64, digestive visits comprised the highest share in 2022 (16.7%), increasing by 0.8 PP from 2017 to 2022.
For patients ages 65+, circulatory ED visits represented the highest share in 2022 (26.8%), with an overall increase of 0.3 PP from 2017 to 2022.
Most Common Emergency Department Diagnoses, Over Time and By Age
From 2017 to 2022, chest pain was the most common diagnosis for ED visits across age groups, followed by abdominal pain (Figure 4). The primary diagnoses for ED visits have generally stayed constant, with the exception of COVID-19, which rose to the third most common diagnosis in 2020. Among patients ages 18-44, abdominal pain was the highest-volume diagnosis over time, followed by chest pain. The inverse was true for patients ages 45-64. For patients ages 65+, other chest pain and urinary tract infections remained the most common complaints, with syncope and collapse surpassing chronic obstructive pulmonary disease with acute exacerbation in recent years.
Given that circulatory conditions have increased in share of ED visits across age groups, we analyzed the most common cardiac diagnoses in the ED over time. From 2017 to 2022, hypertension was the most common cardiac diagnosis in the ED across age groups (Figure 5). The other most common diagnoses have also remained consistent, with hypertensive heart disease with heart failure, hypertensive chronic kidney disease and non-ST-elevation myocardial infarction (i.e., mild heart attack) consistently ranking second, third and fourth. Among patients ages 18-44, pulmonary embolism was the second most common diagnosis from 2017-2021 but dropped to fifth most common in 2022. Conversely, for patients ages 45-64 and 65+, the most common cardiac diagnoses have remained largely constant, with some changes in rank year-over-year.
While no singular trend is driving changes in ED utilization over time, cardiac, behavioral health and genitourinary conditions have seen an increase in their share of ED visits, while the share of respiratory conditions in the ED has declined. Even minor shifts in the reasons for ED utilization can help signal broader changes in disease burden.
Closely analyzing the changes in emergent conditions that patients are presenting with over time is crucial for proactive healthcare responses to emerging patient needs and preventing major public health crises, rather than being reactive, which continues to remain the status quo in the U.S. healthcare system.
Just as investments by biopharmaceutical manufacturers signal changing disease burden (e.g., growing investments in oncology, cardiology and immunology), ED utilization trends present real-time evidence of shifts in patient demand and emerging disease burden.6 Understanding these trends can inform resource allocation, preventive measures, and healthcare policy aimed at improving patient outcomes and mitigating potential crises in the future.
Thanks to Colin Macon and Katie Patton for their research support.






















.png)

















.png?width=171&height=239&name=2025%20Trends%20Report%20Nav%20(1).png)