Service Line Intelligence
2026Behavioral Health Report
Katie Patton•Clara Petrucelli•Maggie Jackson•Austin Miller•Allison Oakes, Ph.D.
Service Line Intelligence Report
America's Preeminent Public Health Challenge
The ongoing behavioral health crisis – encompassing mental illness and substance use disorders – is one of the most pervasive and unresolved healthcare issues in the U.S.
Nearly one in four American adults live with a mental illness, and more than 48,000 people die by suicide each year.
The economic burden is equally staggering. The total cost of behavioral health conditions in the U.S., including healthcare utilization, lost wages, criminal justice encounters and premature deaths, exceeds $300B annually.
Emerging trends suggest that the behavioral health crisis will likely intensify and increasingly affect younger populations.
Applying an Economic Framework to Study Behavioral Health Trends
For decades, the U.S. health economy has operated as if the fundamental rules of economics — demand, supply and yield — do not apply. However, the U.S. healthcare system is what game theorists call a “negative-sum game,” and the rules of that game are immutable. This reality impacts every health economy stakeholder.
Demand
Primary Data Source: National All-Payer Claims Dataset
Supply
Refers to the various providers of health services ranging from hospitals and physician practices to retail pharmacies, new entrants and virtual care platforms.
Primary Data Source: Provider Directory
Yield
Refers to the intersection of demand and supply (i.e., negotiated rate) and is also influenced by market factors such as policy regulations and reimbursement incentives.
Primary Data Source: Health Plan Price Transparency Dataset
Key Findings at a Glance
62.6%
Increase in behavioral health utilization from 2018 to 2024
176.1%
Increase in drug- & alcohol-induced mortality rate since 1999
$477.5B
Estimated annual cost of untreated mental illness in 2024
27.3%
National mental health professional adequacy rate in 2025
.png)
Demand
The U.S. Behavioral Health Crisis Did Not Subside With the End of the Pandemic — It Was Further Amplified
.png)
23.4%
Adults with any mental illness in 2024
1-in-3
Young adults ages 18–25 with any mental illness in 2024
89.3%
Growth in utilization related to anxiety disorders from 2018 to 2024
65.6%
Proportion of telehealth volume attributed to behavioral health in 2024
Key Research Questions
QUESTION 1
How are behavioral health prevalence and mortality changing?
QUESTION 2
How does behavioral health impact different patient populations?
QUESTION 3
How is behavioral health medication use changing?
What's in the Report
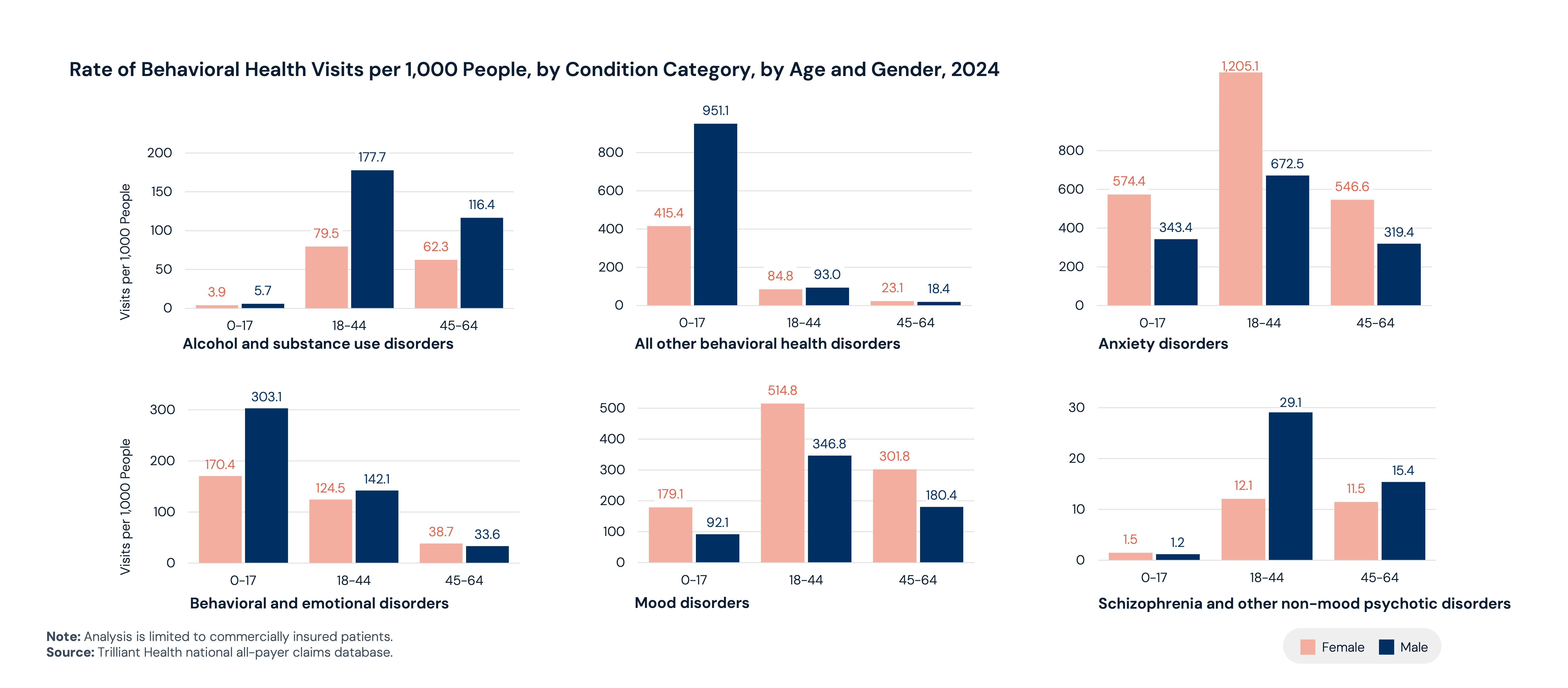
Increasing behavioral health prevalence is concentrated among young adults: Adults ages 18–25 continue to exhibit the highest prevalence of any mental illness (33.2%) and serious mental illness (15.9%), though rates have declined since 2021. As of 2024, anxiety disorders among women ages 18-44 represents the highest behavioral health utilization category (1,205.1 visits per 1,000 people). In contrast, adults ages 26–49 have experienced increases in nearly all mental health and substance use disorders (SUD), with the rate of any mental illness increasing by 1.2 PP and 0.9 PP for co-occurring any mental illness and SUD from 2021 to 2024.
Multiracial individuals demonstrate the most intense behavioral health need: Multiracial individuals have the highest prevalence across major behavioral health conditions, including any mental illness (35.5%), compared to 25.1% of White and 20.9% of Black individuals. Multiracial individuals also have the highest SUD prevalence (24.9%) compared to White (18.5%) and Black (18.3%) individuals.
Sharp increase in drug- and alcohol-induced deaths driven by adult men: Drug- and alcohol-related mortality is higher among men than women, ranging from 2.2x to 2.9x across age groups. Over the past two decades, the drug- and alcohol-induced mortality rate has increased substantially among men ages 18–44 (114.7%), 45–65 (106.9%) and 65–84 (118.7%). Among adolescents, males have the highest intentional self-harm mortality rate, increasing by 45.2% between 2004 and 2024.
Behavioral health accounts for the majority of telehealth use: Telehealth for the treatment and management of behavioral health conditions has emerged as a substitute for in-person care. Since 2018, the proportion of telehealth volume that is attributed to behavioral health has increased from 18.4% to 65.6%.
Stimulants show fastest growth among behavioral health medications: Between 2018 and 2024, the share of patients taking stimulants increased the most (53.3%), followed by antipsychotics (45.4%). However, anxiolytics represent the medication class with the highest overall patient volume.
.png)
Supply
The Behavioral Health Workforce Is Not Equipped to Meet Demand — and the Gap Is Widening
.png)
27.3%
National mental health professional adequacy rate in 2025
99,780
FTE shortfall projected in mental health counseling by 2038
34.3%
Share of behavioral health medications prescribed by allied health providers, exceeding PCPs and psychiatrists
83%
Behavioral health providers reporting burnout in 2023
Key Research Questions
QUESTION 4
What are the trends in behavioral health provider supply?
QUESTION 5
How are novel treatment paradigms and technologies influencing the behavioral health market?
What's in the Report
Over half of large metros have a psychiatrist shortage: Nationally, there are approximately 10,000 people per one psychiatrist. Across CBSAs with populations over 1M, 56.9% are in a shortage relative to this benchmark. For example, while San Francisco, CA has a relative surplus of 541 psychiatrists, Atlanta, GA has a deficit of 348 psychiatrists.
Mental health professional shortage areas span every U.S. state: The percent adequacy of mental health professionals is 27.3% as of 2025, ranging from 5.7% in West Virginia to 52.3% in New Jersey.
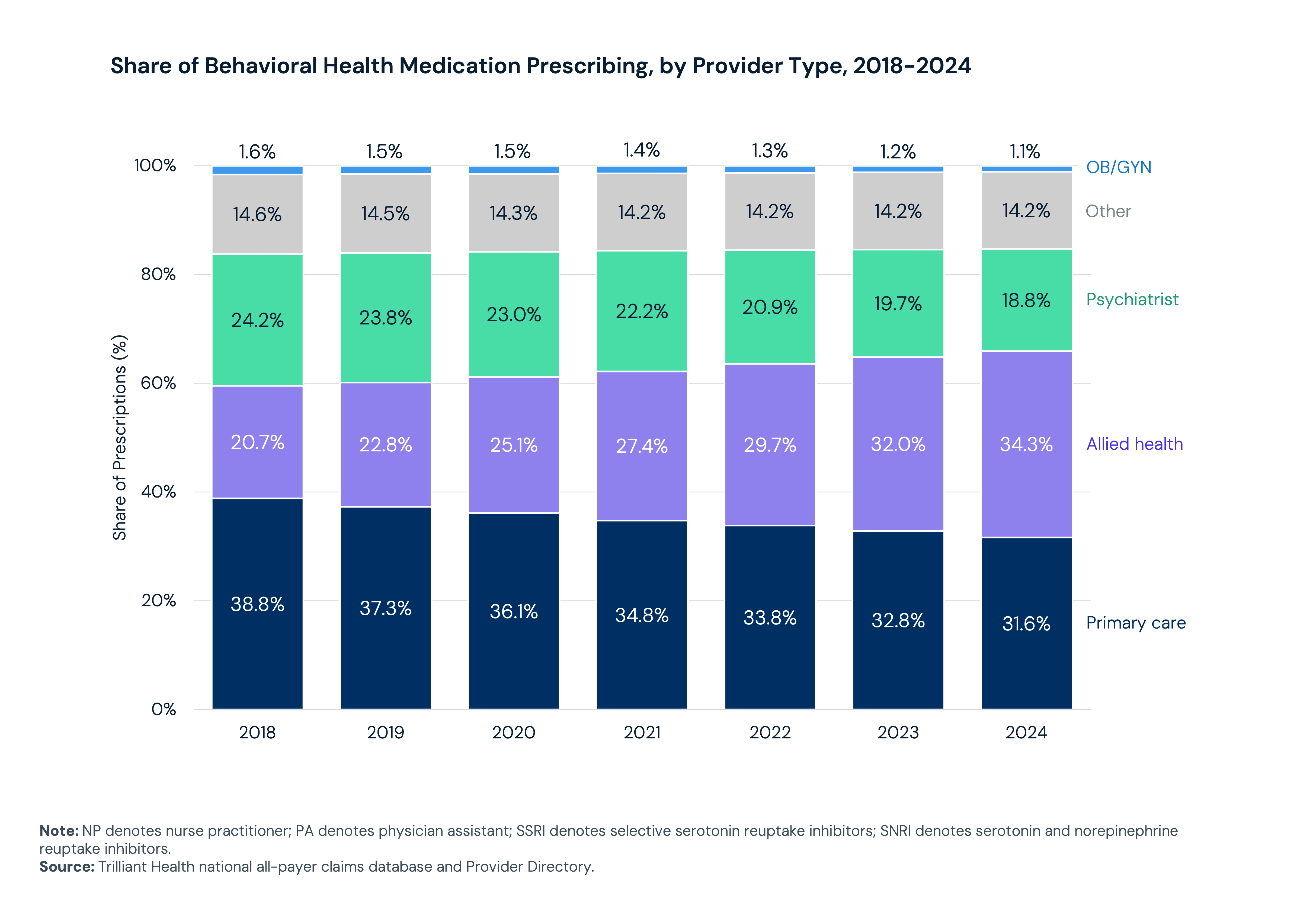
Allied health providers are managing a growing share of behavioral health prescription volume: Prescribing patterns for SSRIs, SNRIs, mood stabilizers and stimulants have shifted substantially in recent years. From 2018 to 2024, allied health providers (i.e., NPs and PAs) became the most common prescribing provider type, increasing from 20.7% to 34.3% of total prescription volume.
Increase in ABA therapy highlights behavioral health vulnerabilities: Since the introduction of new CPT codes in 2019, ABA visit volume has increased substantially across all payer types, reaching a growth rate of 309.2% in 2025.
Yield
The Nature of the U.S. Healthcare System Is Fundamentally Misaligned With Providing High-Value Care to Behavioral Health Patients
$477.5B
Estimated cost of untreated mental illness to the U.S. economy in 2024
65.2%
Percent of adults with mental health needs who cite cost as a barrier to treatment
7x
Variance in commercial negotiated rates for psychotherapy for the same CPT code
Key Research Questions
QUESTION 6
How does behavioral health impact overall healthcare costs?
QUESTION 7
What is the policy landscape in behavioral health?
QUESTION 8
How do prices compare for common behavioral health services?
What's in the Report
Annual economic burden of untreated mental illness exceeds $477B: Untreated mental illness cost the U.S. economy an estimated $477.5B in 2024 and is projected to exceed $1.3T annually by 2040. Most projected costs are attributed to premature death ($911.9B) and workforce productivity losses ($252.3B) including unemployment, absenteeism and presenteeism.
Cost is a primary barrier to accessing behavioral health services: Cost remains a major barrier to behavioral health treatment, cited by 65.2% of adults with unmet mental health needs and 45.3% with substance use disorders. In addition, many also report insufficient insurance coverage.
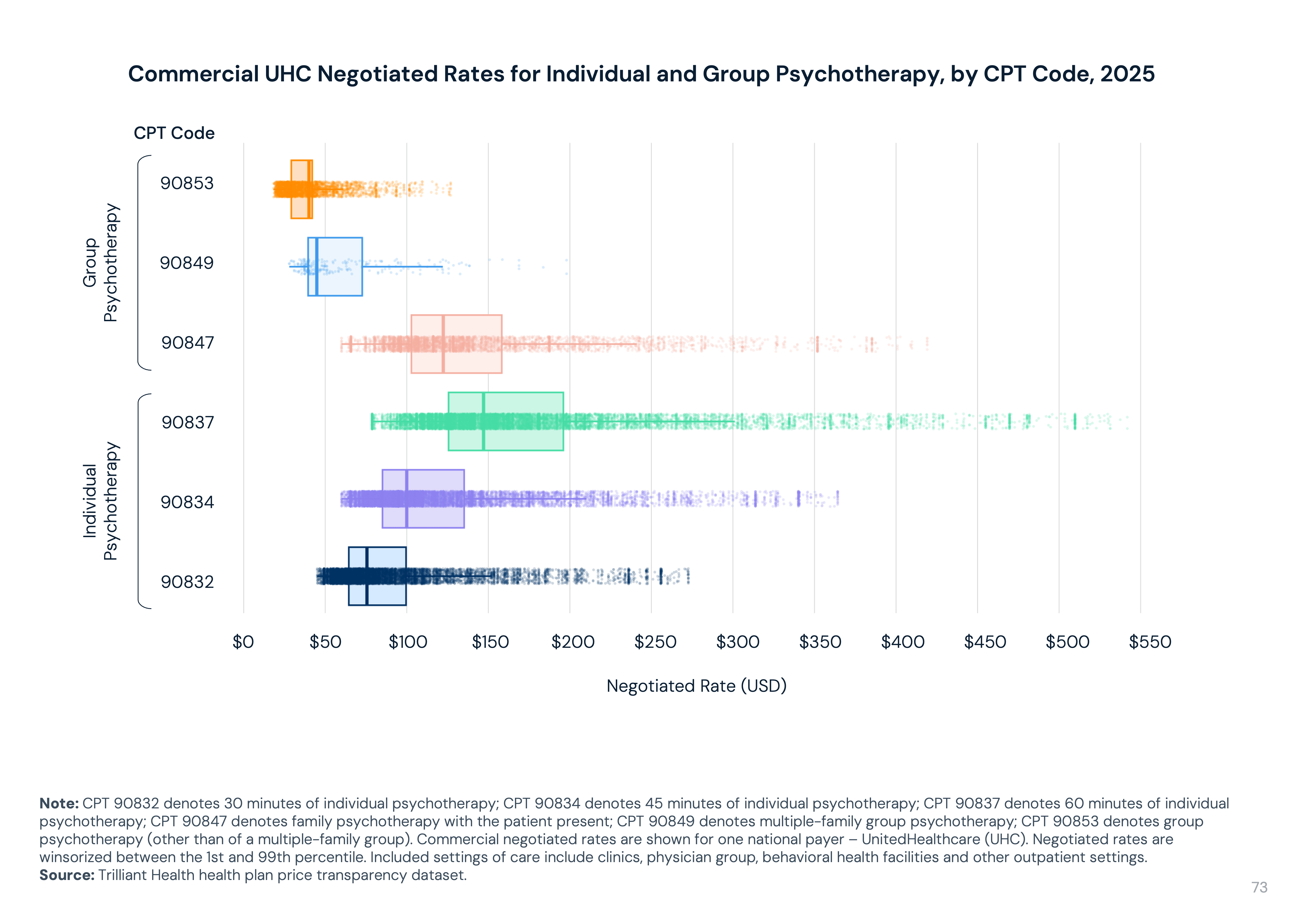
Psychotherapy negotiated rates vary by up to 7x: Commercial negotiated rates for UnitedHealthcare for individual and group psychotherapy codes vary by up to 7x. For example, the median negotiated rate for CPT 90837 (individual psychotherapy) is $147 but ranges from $78 to $542.
“Behavioral health in the U.S. is not a peripheral concern, a niche service line or a problem on the horizon. It is a defining force shaping the demand for care, the capacity of our workforce and the financial performance of every part of the health economy.”
— Allison Oakes, Ph.D. · Chief Research Officer, Trilliant Health
.png)
Conclusion
Stakeholder Imperatives for Action
.png)
Key Imperatives by Stakeholder
Providers
- Establish and maintain a consistent relationship with behavioral health patients to support continuity of care.
- Develop awareness of mental health risk factors and proactively monitor for changes in mood or behavior.
- Understand high-value care pathways to ensure patients engage in timely and appropriate treatment.
Payers
- Ensure broad coverage and network adequacy for behavioral health providers.
- Design reimbursement structures that incentivize measurement-based care and improved clinical outcomes rather than volume of services.
- Identify and proactively manage members with severe mental illness or SUD.
Life Sciences
- Advance development of novel pharmacologic treatments that address unmet needs.
- Partner with providers to improve screening, diagnosis and guideline-concordant treatment.
- Demonstrate clinical and economic value through real-world evidence, including impact on symptom control, adherence and total cost of care.
Employers
- Offer and maintain benefits to ensure employees can access timely, evidence-based services.
- Assess and mitigate organizational factors, such as workload, job strain and lack of flexibility.
- Provide clear and understandable incentives for employees to avoid low-value providers, informed by health plan price transparency data.
Patients
- Establish and maintain a consistent relationship with a behavioral health provider.
- Engage in shared decision-making with providers to understand therapy options, medications and expected outcomes.
- Identify individual risk factors and recognize triggers that may worsen symptoms or lead to relapse.
Policymakers
- Strengthen and enforce mental health parity requirements.
- Support training, loan repayment and scope-of-practice policies to grow and diversify the behavioral health workforce.
- Promote care delivery and payment models that support integration of behavioral health into primary and specialty care.
.png)
Service Line Intelligence | BEHAVIORAL HEALTH
Read the Full 2026 Behavioral Health Report
ABOUT THE REPORT
84 Pages | PDF Download
About Trilliant Health
.png)






















.png)

















.png?width=171&height=239&name=2025%20Trends%20Report%20Nav%20(1).png)
